
What’s the true cause of racial health disparities in America?
 Statistics generally indicate, African- Americans suffer worse health outcomes than Anglo-Americans. African-Americans are 77% more likely to be diagnosed with diabetes than their white peers. African-Americans, especially woman, average the highest blood pressures compared to almost all other groups in the world. Black infants die at over twice the rate of white infants in the United States. Black moms die during or in the first year after childbirth three times more often than white moms (44/100,000 for blacks vs. 13/100,000 for whites). It’s hard to argue with stats like those.
Statistics generally indicate, African- Americans suffer worse health outcomes than Anglo-Americans. African-Americans are 77% more likely to be diagnosed with diabetes than their white peers. African-Americans, especially woman, average the highest blood pressures compared to almost all other groups in the world. Black infants die at over twice the rate of white infants in the United States. Black moms die during or in the first year after childbirth three times more often than white moms (44/100,000 for blacks vs. 13/100,000 for whites). It’s hard to argue with stats like those.
It’s Not Genetics
The reason for the difference in health and mortality among the races has been debated for over a hundred years. In 1899, William Du Bois wrote that differences in health outcomes for African-Americans had more to do with Anglo-Americans “social advancements” and the “vastly different conditions” in which people of color lived compared to whites. Others of his time argued that these differences were due largely to biological differences between races. Since the discovery of the double helix in the 1950s, billions in funding has gone into researching differences in DNA that might predispose African- Americans to higher rates of disease and lower life expectancy, but little has been discovered to support genes as the cause.
A person’s genetic make-up doesn’t make him or her more likely to be shot by police while unarmed like what happened to Michael Brown in the city of Ferguson, Missouri in 2014. More white people are killed every year by police in this country, but African-Americans make up only 13% of the US population. When you do the math, you find that black people are about three times more likely to be killed by ‘legal force’ in the US than whites. Though statistically improbable that you will be killed by the police, a recent study has found that police killings of unarmed African-Americans have adverse effects on the mental health of all black adults in the general population. Not surprisingly, living in an environment that is perceived as dangerous, is bad for an individual’s mental and physical health.
What About Social Determinants of Health?
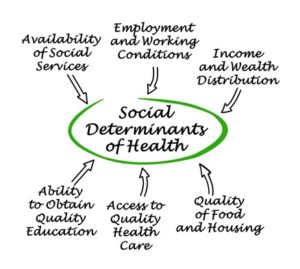 Social determinants of health – defined by the authors of Healthy People 2020 as “conditions in the environments in which people are born, live, learn, work, play, worship, and age that affect a wide range of health, functioning, and quality-of-life outcomes and risks” are the true makers or breakers of a healthy life, and the human genome has much less to do with it than most people think. The same goes for individual risk factors. The World Health Organization states that social determinants of health are the “fundamental drivers” of health disparities around the globe.
Social determinants of health – defined by the authors of Healthy People 2020 as “conditions in the environments in which people are born, live, learn, work, play, worship, and age that affect a wide range of health, functioning, and quality-of-life outcomes and risks” are the true makers or breakers of a healthy life, and the human genome has much less to do with it than most people think. The same goes for individual risk factors. The World Health Organization states that social determinants of health are the “fundamental drivers” of health disparities around the globe.
But if health comes down to your social situation – where you were born, raised, educated, and live, then why do educated African- American mothers who earn a good income, live in a good neighborhood, and have a great support system, still die more often than their less-educated, lower socio-economically matched white peers? This information often leads people to lean towards genetic make-up as the underlying cause, but there’s another explanation. It’s not just where you were born, raised, and educated – it’s also very much about how you are treated.
More specifically, health is about how social structures intentionally or unintentionally create pervasive conditions that prejudice against minorities. Structural inequality is defined as a condition where one category of people is attributed an unequal status in relation to other categories of people. These social inequities manifest as health disparities in those groups that are disadvantaged. The mechanism of action is stress.
Stress Comes in Many Forms

Stress has been described by some as the most common cause of human illness. Any kind of stress counts – physical stress (poor nutrition, lack of sleep), emotional stress (financial troubles, divorce) and of course, toxic stress – often caused simply by feeling judged by, unable to keep up with, or ‘less than’ your peers. Chronic stress can have a massive effect on health outcomes (especially when experienced in childhood) and racism is one of the most unrecognized forms of chronic stress that minorities are dealing with today.
Recent studies found that discrimination is linked to a wide range of health outcomes, such as less stage four sleep (a major health indicator), abdominal fat (a serious threat to longevity), heart disease, diabetes, and for women: fibroids and breast cancer.

Access to healthy food, clean water, and healthcare are obvious basic needs. But even after basic material needs are met, African-Americans still suffer worse health outcomes than their white peers. This suggests a greater need for more focus on the social structures that create disparities in how African-Americans are treated, and ultimately lead to higher levels of stress. Research has demonstrated negative health consequences to perceived discrimination, as well as, actual discrimination.
Essentially, each black person that is unfairly targeted and unfairly treated can negatively affect the health of others. To achieve health equity and create a healthy society for all, we must acknowledge injustices caused by racism.
A More Equitable Society
If researchers and doctors want to get serious about creating a more equitable society, where racial health disparities no longer impact America’s declining health, then the issue of discrimination and its impact on chronic, toxic stress needs to be addressed – with more funding for research, more support and services for all minorities, and most importantly, more education for a country whose health status is going in the wrong direction.


